

Sharing is caring: A better index for insights & impact
We're on a mission to measure what matters to community well-being. Use our data to make positive changes where we live, work, and play. Together, we will help more people live better, longer.
2022 state rankings report released September 12, 2023-- Learn more
Mapping measures for meaning
Our interactive map gives you powerful perspective on our data. Go broad, such as comparing your state to others. Or go deep, such as isolating the well-being concerns in your community. And that's only the start.
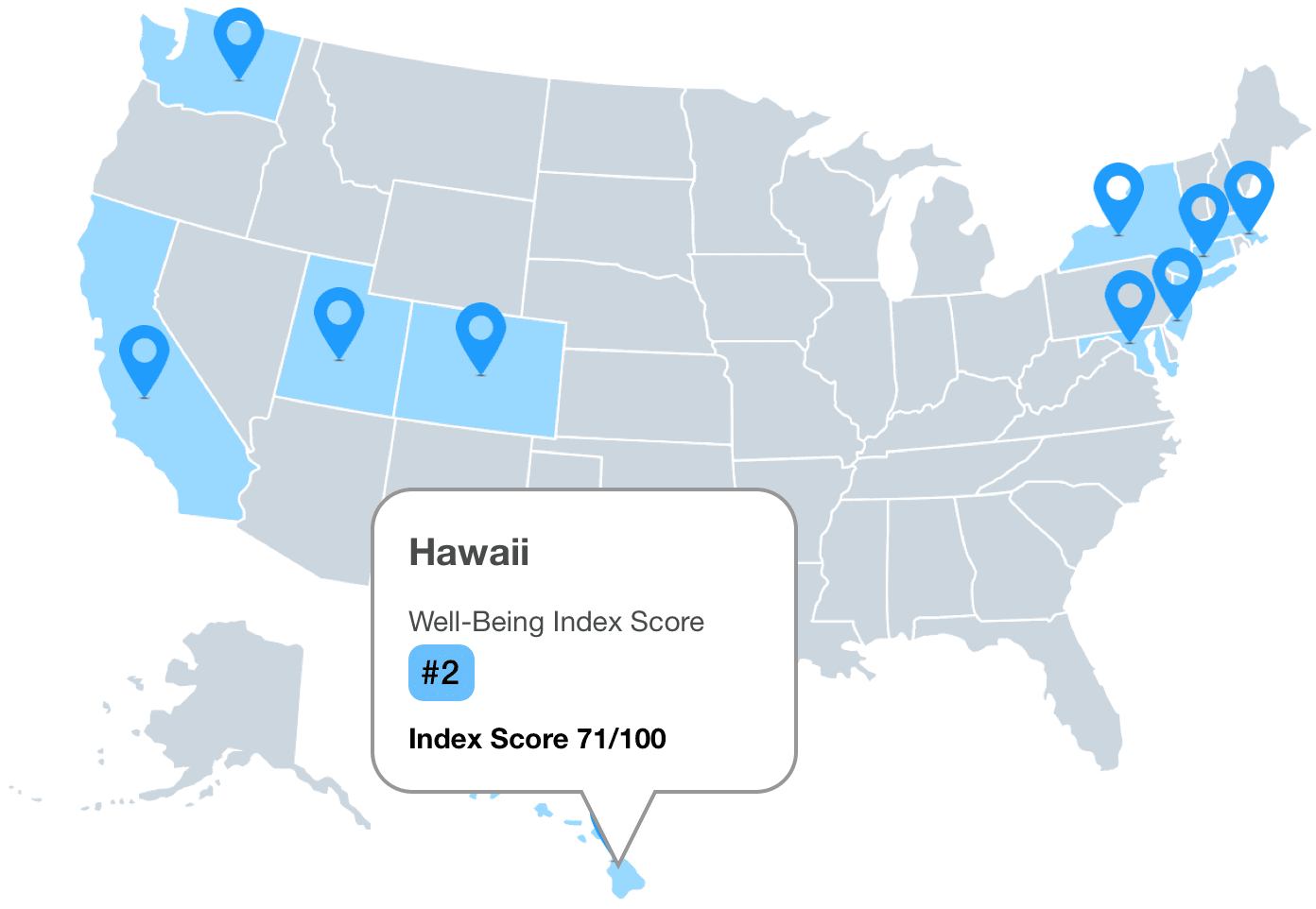
How's the health in your community?
Community Well-Being Index by the numbers
What is the Sharecare Community Well-Being Index?
Our index brings together more than 600 proven health risk factors into a single measure. By combining both individual and social factors, our index uniquely measures well-being across people and places.
We based the index on decades of clinical research, health care leadership, and health economics. We conduct regular surveys within every community in the United States. We then analyze that data and score each community on a scale of 0 to 100. Updated every year, our current index is based on responses from more than 5 million surveys and 600+ social determinants of health.

Physical
Having good health and enough energy to get things done daily

Financial
Managing your economic life to increase financial security and reduce stress

Social
Having supportive relationships and love in your life

Community
Liking where you live and having pride in your community

Purpose
Liking what you do each day and being motivated to achieve your goals
For our partners
A layered approach to understanding the context of a community. Rather than focus only on the result, we can identify the root cause. And that insight sparks real change.
Know your Data
Including both individual risk and social determinant risk for the places your employees live and work
Create Awareness
Democratize the information found, ensuring your employee population and community understand their SDOH circumstances
Integrate
Integrate into benefits configuration, health equity considerations, worksite & built environment, community
Measure Impact
Including how our efforts are augmenting well-being for your employees as well as the community broadly

Data in action
See our index make an impact on community well-being.
Sustainability and its Links to Well-Being
Depression Risk and Financial Health are Intrinsically Connected
Sharecare Community Well-Being Index Finds Broad Improvements in US Metro Areas in 2020 but Substantial Declines for Certain Sub-populations
U.S. Vaccination Rates Slow Amid Rise of Delta Variant
Research & Analysis
Delve into details for your industry or role.




